Overview

he belly isn't the only part of your body subject to middle-age spread. As we get older, the years of walking and standing can cause feet to spread and flatten out as ligaments that support the arch lose their holding power. The result: the condition known as fallen arches, or flat feet. "Keep in mind that we're talking about 26 bones in the foot that are supported by a series of ligaments, muscle tendons and other connective tissue," says Glenn Gastwirth, D.P.M., deputy executive director of the American Podiatric Medicine Association in Bethesda, Maryland. "Over a period of time, the ligaments stretch out or 'give' under the pressure of your weight-especially if you're overweight. So what usually happens is you go shopping for new shoes one day and suddenly realize that you now need a size 8 when you've always worn a size 6. You may think your foot has grown, but what really happens is that the foot has spread out, both in width and length."
Causes
Turning 40 doesn?t necessarily have anything to do with it, but over time you?ve likely engaged in certain activities or developed some unhealthy habits that led to this condition. If you are overweight, you are placing excess burdens on your feet, causing the tendons to strain. Some women experience fallen arches because of weight gain during pregnancy. You also may have damaged these tendons while exercising. If you suffered a serious injury to the foot, you may have weakened the tendons, which can also lead to this development.
Symptoms
Some people have fallen arches, and they aren?t even aware of it, fallen arches are sometimes asymptomatic and do not always cause pain. However, for others, the following symptoms may be present. Foot pain, particularly in the arches or heels, leg or back pain, feet feel tired quickly, swelling in the feet and difficulty moving the feet.
Diagnosis
If your child has flatfeet, his or her doctor will ask about any family history of flatfeet or inherited foot problems. In a person of any age, the doctor will ask about occupational and recreational activities, previous foot trauma or foot surgery and the type of shoes worn. The doctor will examine your shoes to check for signs of excessive wear. Worn shoes often provide valuable clues to gait problems and poor bone alignment. The doctor will ask you to walk barefoot to evaluate the arches of the feet, to check for out-toeing and to look for other signs of poor foot mechanics. The doctor will examine your feet for foot flexibility and range of motion and feel for any tenderness or bony abnormalities. Depending on the results of this physical examination, foot X-rays may be recommended. X-rays are always performed in a young child with rigid flatfeet and in an adult with acquired flatfeet due to trauma.
pes planus orthotics
Non Surgical Treatment
Treatment in adults generally consists of wearing spacious, comfortable shoes with good arch support. Your doctor may recommend padding for the heel (heel cup) or orthotic shoe devices, which are molded pieces of rubber, leather, metal, plastic, or other synthetic material that are inserted into a shoe. They balance the foot in a neutral position and cushion the foot from excessive pounding. For children, treatment using corrective shoes or inserts is rarely needed, as the arch usually develops normally by age 5.
Surgery is rarely needed.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.

he belly isn't the only part of your body subject to middle-age spread. As we get older, the years of walking and standing can cause feet to spread and flatten out as ligaments that support the arch lose their holding power. The result: the condition known as fallen arches, or flat feet. "Keep in mind that we're talking about 26 bones in the foot that are supported by a series of ligaments, muscle tendons and other connective tissue," says Glenn Gastwirth, D.P.M., deputy executive director of the American Podiatric Medicine Association in Bethesda, Maryland. "Over a period of time, the ligaments stretch out or 'give' under the pressure of your weight-especially if you're overweight. So what usually happens is you go shopping for new shoes one day and suddenly realize that you now need a size 8 when you've always worn a size 6. You may think your foot has grown, but what really happens is that the foot has spread out, both in width and length."
Causes
Turning 40 doesn?t necessarily have anything to do with it, but over time you?ve likely engaged in certain activities or developed some unhealthy habits that led to this condition. If you are overweight, you are placing excess burdens on your feet, causing the tendons to strain. Some women experience fallen arches because of weight gain during pregnancy. You also may have damaged these tendons while exercising. If you suffered a serious injury to the foot, you may have weakened the tendons, which can also lead to this development.
Symptoms
Some people have fallen arches, and they aren?t even aware of it, fallen arches are sometimes asymptomatic and do not always cause pain. However, for others, the following symptoms may be present. Foot pain, particularly in the arches or heels, leg or back pain, feet feel tired quickly, swelling in the feet and difficulty moving the feet.
Diagnosis
If your child has flatfeet, his or her doctor will ask about any family history of flatfeet or inherited foot problems. In a person of any age, the doctor will ask about occupational and recreational activities, previous foot trauma or foot surgery and the type of shoes worn. The doctor will examine your shoes to check for signs of excessive wear. Worn shoes often provide valuable clues to gait problems and poor bone alignment. The doctor will ask you to walk barefoot to evaluate the arches of the feet, to check for out-toeing and to look for other signs of poor foot mechanics. The doctor will examine your feet for foot flexibility and range of motion and feel for any tenderness or bony abnormalities. Depending on the results of this physical examination, foot X-rays may be recommended. X-rays are always performed in a young child with rigid flatfeet and in an adult with acquired flatfeet due to trauma.
pes planus orthotics
Non Surgical Treatment
Treatment in adults generally consists of wearing spacious, comfortable shoes with good arch support. Your doctor may recommend padding for the heel (heel cup) or orthotic shoe devices, which are molded pieces of rubber, leather, metal, plastic, or other synthetic material that are inserted into a shoe. They balance the foot in a neutral position and cushion the foot from excessive pounding. For children, treatment using corrective shoes or inserts is rarely needed, as the arch usually develops normally by age 5.
Surgery is rarely needed.
Surgical Treatment

This is rare and usually only offered if patients have significant abnormalities in their bones or muscles. Treatments include joint fusion, reshaping the bones in the foot, and occasionally moving around tendons in the foot to help balance out the stresses (called tendon transfer). Flat feet and fallen arches are common conditions that are in most cases asymptomatic. However, in patients who do have symptoms, treatments are available that can help reduce pain and promote efficient movement. Orthotic devices are well recognised as an excellent treatment and podiatrists can offer these different treatment modalities as individualised treatments for patients.
After Care
Patients may go home the day of surgery or they may require an overnight hospital stay. The leg will be placed in a splint or cast and should be kept elevated for the first two weeks. At that point, sutures are removed. A new cast or a removable boot is then placed. It is important that patients do not put any weight on the corrected foot for six to eight weeks following the operation. Patients may begin bearing weight at eight weeks and usually progress to full weightbearing by 10 to 12 weeks. For some patients, weightbearing requires additional time. After 12 weeks, patients commonly can transition to wearing a shoe. Inserts and ankle braces are often used. Physical therapy may be recommended. There are complications that relate to surgery in general. These include the risks associated with anesthesia, infection, damage to nerves and blood vessels, and bleeding or blood clots. Complications following flatfoot surgery may include wound breakdown or nonunion (incomplete healing of the bones). These complications often can be prevented with proper wound care and rehabilitation. Occasionally, patients may notice some discomfort due to prominent hardware. Removal of hardware can be done at a later time if this is an issue. The overall complication rates for flatfoot surgery are low.



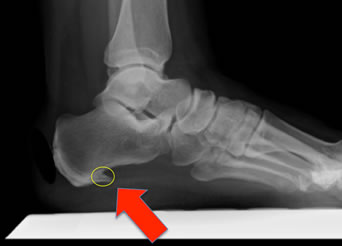
 Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.
Morton's neuroma, also called Morton's metatarsalgia, Morton's disease, Morton's neuralgia, Morton metatarsalgia, Morton nerve entrapment, plantar neuroma, or intermetatarsal neuroma is a benign (non-cancerous) growth of nerve tissue (neuroma) that develops in the foot, usually between the third and fourth toes (an intermetatarsal plantar nerve, most commonly of the third and fourth intermetatarsal spaces). It is a common, painful condition.
 Overview
Overview
 Though a bunion is often described as a painful bump, this condition is much more complex than a simple bump on the side of the toe. X-rays show the true nature of the deformity and are used to help in the decision making process. Ranges of motion of joints associated with the toe are also performed to assess the deformity. There are many procedures for correcting a bunion and choosing the right one based on the examination increases the chance of success. The procedure performed on one person may not be the procedure required to give another a good result. In general, more severe bunion deformities require more extensive surgery and more extensive post-operative limitations. It is very important to note that the same instability and incorrect motion that causes a bunion also causes degeneration of the joint surfaces (osteoarthritis). Correction of the bunion cannot repair the damage done within the joint and continued pain from that separate process may occur. Realigning the joint may slow the damage within the joint and improve motion, but it may not alleviate all pain.
Though a bunion is often described as a painful bump, this condition is much more complex than a simple bump on the side of the toe. X-rays show the true nature of the deformity and are used to help in the decision making process. Ranges of motion of joints associated with the toe are also performed to assess the deformity. There are many procedures for correcting a bunion and choosing the right one based on the examination increases the chance of success. The procedure performed on one person may not be the procedure required to give another a good result. In general, more severe bunion deformities require more extensive surgery and more extensive post-operative limitations. It is very important to note that the same instability and incorrect motion that causes a bunion also causes degeneration of the joint surfaces (osteoarthritis). Correction of the bunion cannot repair the damage done within the joint and continued pain from that separate process may occur. Realigning the joint may slow the damage within the joint and improve motion, but it may not alleviate all pain.
